- Timeless Autonomy
- Posts
- Paying for Brainpower: The Evolution of Longitudinal Care Reimbursement
Paying for Brainpower: The Evolution of Longitudinal Care Reimbursement
ACCESS, GUIDE, APCM, and more!

**Disclaimer: All opinions and ideas expressed in this article are solely mine and none represent a recommendation or should be viewed as advisement of any kind to anyone to do anything.*
Policy Pulse
The Cognitive Comeback | Reimbursing Brain Power
I was thinking about various policy changes and models rolled out by CMS and the Innovation Center over the past decade.
They’ve created additional codes for cognitive work and coordination of care, such as chronic care management, principal illness navigation, caregiver training, advance care planning, and much more. We have needed to pay for these types of activities for forever. Not paying for them, plus fee-for-service incentives, have led to little longitudinal care and failures of population health in America.
While adoption of advanced primary care is variable, it’s working!
But there’s this other dynamic happening in parallel.
CMS is creating codes like the Advanced Primary Care Management (APCM) codes, which essentially allow practices to simplify care management tracking and bill one monthly code that includes a number of these “cognitive codes.”
It can lead to higher overall primary care practice reimbursement and encourage these activities to be performed, especially for practices who aren’t participating in value-based care arrangements.
For practices who have operationalized the various codes and services, it can potentially yield lower revenue by the nature of bundling of the codes.
Of course, those at full financial risk are typically not concerned about code volumes. They are concerned about engaging their attributed population and preventing unnecessary and avoidable healthcare utilization. Their reimbursement isn’t determined by billable units. The administrative time it takes to track and comply with the rules around use of these codes is often determined to be “the juice is not worth the squeeze.”
The “So What”
Policymakers began reimbursing for services that are now seen as valuable and worth paying for. 👏
At the same time, I see them trying to address two other dynamics.
The first is making adoption more widespread by simplifying and bundling related “cognitive” services.
The second is proactively mitigating the risk of the overutilization of the same services by simplifying and bundling related “cognitive” services.
Let’s look at how this applies to two models—one active, one beginning this year.
The GUIDE Model: A Condition-Specific Longitudinal Care Model
Let’s look at the Guiding an Improved Dementia Experience, or GUIDE Model, for dementia and its code for the Dementia Care Management Payment (DCMP). It’s meant to replace all these services below. 👇️
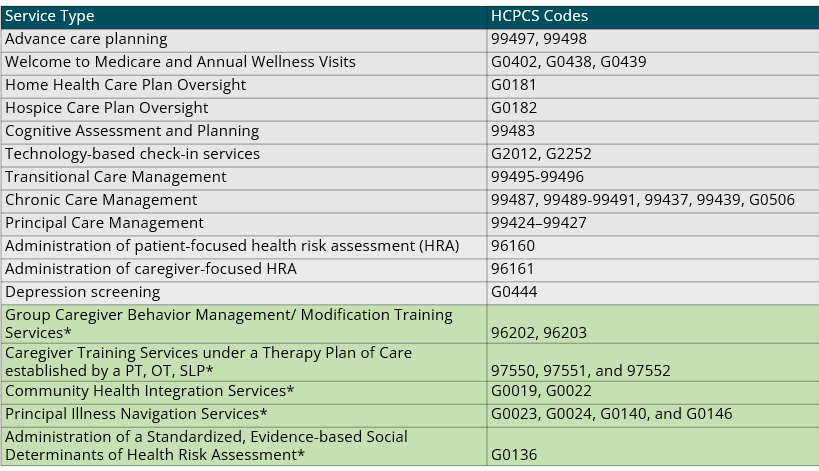
Medicare Physician Fee Schedule Services covered under the Dementia Care Management Payment in the GUIDE Model
Note: this doesn’t stop another provider from billing the above codes for a patient in GUIDE (assuming the other provider is not a GUIDE “Partner Organization”), and the GUIDE Participant isn’t penalized for “substitute spend” if that does happen. (Like in ACCESS, which we’ll talk about next.)
GUIDE is structured in a way that’s not necessarily meant to save money, although CMMI hopes it does. Dementia patients are thought to be under-utilizing upstream services significantly, leading to high downstream costs and high risk of institutionalization.
The Guide Model is meant to improve quality of care and life for patients living with dementia and their unpaid caregivers. It’s a Biden-era model that the Trump Administration’s CMMI Director Abe Sutton retained.
GUIDE aligns patients voluntarily, and patients with ICD.10 coded diagnoses for dementia can be referred ongoing by anyone at any time (think discharge planners, home health agencies, PCPs, therapists, etc). These patients are often not getting the care management and coordination of care they need in fee-for-service. They and their caregivers often end up in ERs and eventually skilled nursing facilities because they don’t know what else to do. The GUIDE Model is meant to address this.
Participants in the model can only “lose” a small amount of their payment based on poor quality performance, so there’s no true, significant risk. CMMI even provides a helpful data dashboard to each Participant so they identify actionable insights and can track their performance, perhaps without needing to secure additional outside analytics solutions .
The ACCESS Model | A Model testing Recurring, Outcome-Aligned Payments for Managing a Patient’s Qualifying Condition
Now let’s look at the Advancing Chronic Care Through Effective, Scalable Solutions (ACCESS) Model. ACCESS participants bill the g-codes to provide monthly support for a bucket of conditions. The same Medicare Part B provider can’t bill any FFS codes for a patient if they are billing the ACCESS code.
ACCESS is the first model to withhold significant reimbursement per patient from the Participant. 50% of reimbursement will be paid retrospectively based on outcomes and the presence or absence of “substitute spend.”
Then CMMI is paying the ACCESS orgs a low annual fee meant to encourage innovation. This will limit the types of organizations who can successfully implement the model, and that’s by design.
Notable Differences
GUIDE and ACCESS both feature monthly payments for managing a condition.
Unlike the approach taken in GUIDE, CMMI is paying the referring and coordinating provider about $100 per patient per year that’s enrolled in ACCESS. The combined payments to the ACCESS org and the referring/coordinating provider are now about on par with the GUIDE payment. There’s nothing like that in GUIDE, but CMMI surely knows it’s hard for primary care practices to effectively manage many patients with dementia and other parts of the healthcare continuum are already looking for places to refer them.
(Note: GUIDE also includes up to $2500 per year reimbursement for respite services for qualifying beneficiaries, but that’s out of scope for this post.)
The coordination payment in ACCESS also addresses something else.
If a provider is billing the coordination fee, they are not permitted to bill the “substitute spend” codes. So this could reduce monthly care management, RPM, and additional code utilization. It also includes PT and OT evaluations in substitute spend codes for the MSK track, and has a similar structure for the Behavioral Health track.
Side note from a PT and VBC expert: Thank you to CMMI for changing the policy and allowing therapists to be the referring providers and bill the co-management fee for the MSK track. It was announced this past week on a webinar. This is a gamechanger for therapists. I Just hope they realize the layers of opportunity here—this is a meaningful inroad into ACO partnerships!
In ACCESS, note CMMI is incentivizing the referring provider to receive and incorporate information from the ACCESS org into the patient’s overall care plan. I see this as an investment so ACCESS orgs have enough patient volume to create a margin with CMMI’s “disciplined” reimbursement rates for what effectively will be digital health access for Medicare beneficiaries.
ACO Primary Care Flex Model | Prospective Primary Care Payments for Certain MSSP ACO Participants
While out of scope for this post, The ACO Primary Care Flex Model is another model that bundles primary care services into a payment for Participants. This is relatively similar to how ACO REACH determines prospective payments for primary care.
This is somewhat different from the APCM, GUIDE, and ACCESS examples because this payment is made as part of participation in the model. Codes billed that overlap are “zeroed out” and not reimbursed. I’m oversimplifying here to give a 30,000 foot view only. There’s lots of information available if you want to dig in.
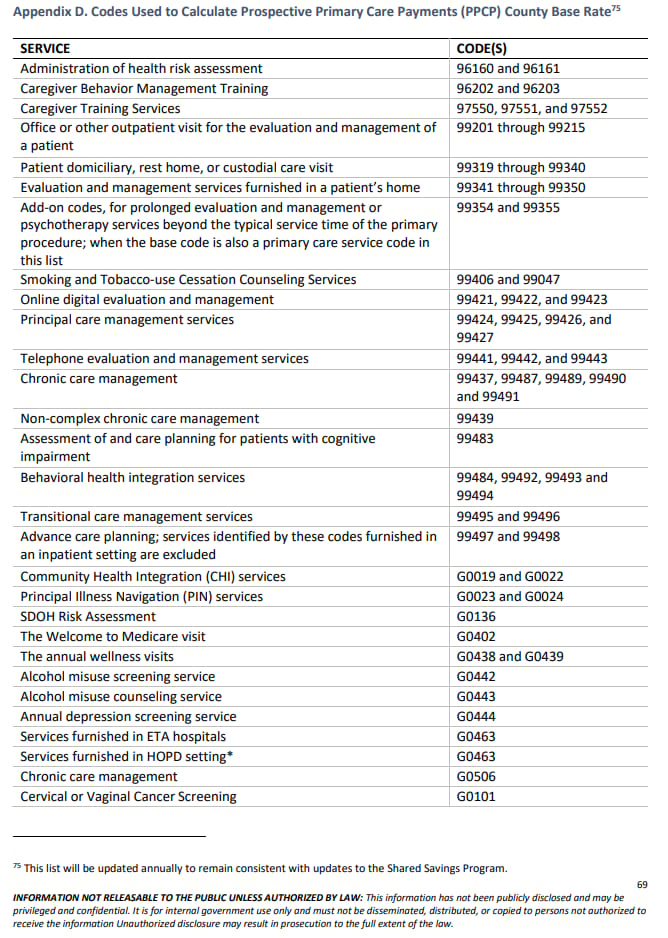
Here are the codes used to determine the base rate, from the ACO Primary Care Flex RFA:
I wrote about ACO Primary Care Flex in 2024 if you want to check it out👇️
Here’s My Point
CMS post-Affordable Care Act changed direction and began to reimburse for the “cognitive work” of primary care teams.
They have added to the list of available services and codes.
They are also building a primary care “bundle” code, which they may add to further.
Then CMMI creates models that “bundle” codes for cognitive services.
But here’s the thing:
Cognitive services, prevention activities, proactive outreach—these are not services we should be trying to limit, right? They aren’t causing runaway spending.
You know what is? High cost biologics, avoidable and preventable hospitalizations, avoidable surgeries, avoidable imaging….
CMS wants to prevent overuse of codes, but we are focused heavily on the low cost and high-value codes.
Sometimes I wonder—why don’t we just pay primary care more and differently across the board? Yes, it will require reducing reimbursement for other Medicare Part B services. I suppose CMS may think that will just lead to more volume of those services if their reimbursement drops?
They may also be afraid of the backlash after finalizing G2211, which Congress required CMS to hold on implementing for several years because it was going to reduce reimbursement to specialists (it also reduced reimbursement to PT and OT, which is crazy—they are already underpaid 😠 ).
On that note, I’ll leave you with this tidbit I read somewhere this week. If I find the link, I’ll add it to the online post version later. 👇️ 😁
There was so much noise around the add-on complexity code for longitudinal care, G2211.
The predictions of primary care provider utilization of this code were very high. Turns out? Specialists (those who can bill E and M codes) are using the codes more than PCPs. I’m being a cynic and generalizing here, but I don’t know a lot of specialty physicians who own longitudinal care like primary care providers do.
The Future of Primary Care: Team-Based, Higher-Paid, Prospectively-Paid, with Longitudinal Accountability
I’ll venture to say we are realistically 5-10 years away from the widespread norm of paying at least our primary care provider teams prospectively, not just in CMS Innovation Center models. We might see the same for certain specialty care, like for those treating dementia and ESRD patients, also.
The work is heavily overweight on care that requires communication, connection, patient engagement, patient outreach. Figuring out how to price and bill for those services individually seems like an intractable problem.
The X-factor will be what role technology plays outside of human interaction. This is really what ACCESS is testing in my opinion. Put technology in the extended care team and give it wide freedom to innovate. Where it will fit and how it will be reimbursed in the future will surely be informed by the results of ACCESS.
This Week, Try This
Please consider attending the webinar I’m on with Dr. Marc Gruner, Dr. Christian Penn, and Dr. Ben Schwartz on the ACCESS Model on Thursday, March 12th.
Check out Dr. Penn’s Substack article here.
Check out some classics from the Timeless Autonomy archives! 👇️
Check out my Medbridge webinar on the Transforming Episode Accountability Model (TEAM) for clinicians! 👇️ It’s free with a Medbridge subscription or can be purchased as an individual course from Medbridge.
Not a subscriber? Using my link gives you $106 off your subscription for unlimited CEUs with code DanaStrauss. They have a host of different types of CEUs for various clinicians. The subscription is a must for me since N.J. requires live CEUs and Medbridge adds live webinars monthly.
**Disclaimer: All opinions and ideas expressed in this article are solely mine and none represent a recommendation or should be viewed as advisement of any kind to anyone to do anything.*







Reply