- Timeless Autonomy
- Posts
- The Room is Spinning. So is the Billing and Patient Fear
The Room is Spinning. So is the Billing and Patient Fear
How a treatable inner ear condition became a $2 billion diagnostic mess


Table of Contents
|
|
**Disclaimer: All opinions and ideas expressed in this article are solely mine and none represent a recommendation or should be viewed as advisement of any kind to anyone to do anything.*
Policy Pulse
Spinning Its Wheels: How Medicine Keeps Getting Vertigo Wrong
You roll over in bed at 2 a.m. The room lurches. You’re convinced something’s very wrong—like a stroke or something else that feels catastrophic. You head to the ER. Hours and tens of thousands of dollars later, you go home with a diagnosis of "dizziness" or “vertigo” and a prescription for a drug that does absolutely nothing to fix what's wrong (meclizine/Antivert).
I watched this or something similar play out dozens of times as a physical therapist. A patient has a general diagnosis of “dizziness” or “vertigo” after a rule out of something neurological and they are given an oral medication and sent home.
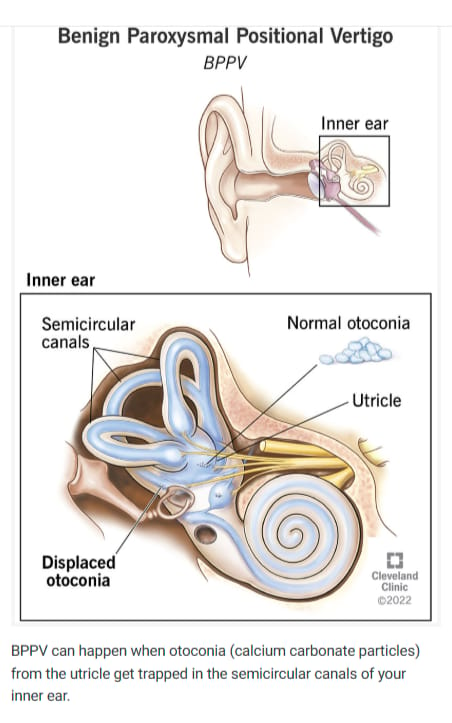
The condition is called Benign Paroxysmal Positional Vertigo (BPPV) and it is almost absurdly treatable. Tiny calcium crystals called otoliths (also known as “otoconia”) drift out of position in the inner ear and trick the brain into thinking the body is spinning. The fix?
A clinician guides your head through a specific repositioning sequence called the Epley maneuver (in the most common presentation of BPPV with a slightly different “maneuver” for the others) and the crystals migrate back where they belong. One visit. Sometimes one treatment. Symptoms gone.
No MRI required. No CT. No overnight admission. No neurologist. No ENT.
I treated BPPV regular in outpatient rehabilitation and even in home health rehabilitation. I’ve since treated multiple family members and friends.
And yet.
It’s the most expensive dizzy spell in medicine.
Healthcare costs associated with diagnosing BPPV alone approach $2 billion per year in the United States, with more than 65% of patients undergoing potentially unnecessary diagnostic testing or interventions (and that’s from a 2017 article, so let’s assume it’s a low estimate of dollars spent). Unnecessary diagnostic procedures have been reported in more than 65% of BPPV patients even in advanced countries, including rates of 70% for MRI and 45% for CT.
Why? Some hypotheses:
Because vertigo can feel terrifying, and terror in medicine often defaults to imaging.
Because stroke and BPPV can look similar to an undertrained eye.
Because medical education gives vestibular disorders roughly the attention of a footnote.
And because fee-for-service payment systems reimburse the scan, not the skillful bedside maneuver. That maneuver is commonly perfected by trained physical therapists.
The drug most commonly prescribed for BPPV, meclizine (Antivert), is a particular frustration. It suppresses vestibular signals. It sedates the complaint. It does not and cannot move the otoconia. Patients taking it aren't getting better. Sometimes the crystals drift back to where they belong on their own. Sometimes the crystals remain exactly where they don't belong, and the clock runs out on days the patient could have been functional, working, and not terrified.
Delayed diagnosis and treatment of BPPV is associated with increased rates of anxiety and depression, lost workdays, inappropriate use of emergency resources, and reduced quality of care. These are the kind of outcomes that show up in utilization data, readmission rates, and disability claims.
What we’re not teaching
Ask most ER physicians (or primary care providers in urgent care and primary care) to perform a Dix-Hallpike (the bedside test that can diagnose BPPV in under two minutes) and many will hesitate. It's not complicated. It requires tilting the patient's head at a specific angle and watching for characteristic eye movement. But it takes practice and pattern recognition that a brief residency mention doesn't build.
Physical therapists, by contrast, evaluate and treat BPPV regularly. It is one of the rare conditions in PT where full resolution in a single session is not just possible but common. The irony is that patients often reach us only after exhausting every expensive wrong turn the system sent them on first. Another great reason for PTs to work as the norm in primary care, urgent care, and emergency rooms.
What AI can do right now to help
Here's where it gets interesting. Researchers have developed machine learning models to classify vestibular disorders using patient-reported symptoms alone, achieving 88% accuracy. Why? Because conditions like BPPV can often be diagnosed primarily through what patients describe.
The symptom profile is specific: brief spinning triggered by lying down or turning the head, no hearing loss, no neurological symptoms, no spontaneous vertigo. A dizzy patient describing those features to an ambient listening tool in a busy ER is practically flagging their own diagnosis. A patient saying "the room spins when I roll over, just for a few seconds" is practically self-diagnosing.
Tools that provide ambient AI infrastructure already suggest ICD-10 codes in real time based on what a clinician says aloud. They can hear a patient describe positional vertigo. The technology to flag that pattern and prompt "consider Dix-Hallpike before ordering imaging" is a configuration decision that someone needs to prioritize.
This one is solvable
Value-based care models have an opening here. Treat BPPV as a sentinel condition: high-frequency, low-complexity, wildly over-imaged. Track inappropriate imaging rates. Reimburse the bedside maneuver. Build BPPV recognition into clinical decision support as a default, not an afterthought. Require a Dix-Hallpike before a vertigo-related CT and/or MRI order in low-risk presentations.
Sidenote: The inspiration for this piece was my mother’s visit to the ER this week. They added an MRA to the above-mentioned diagnostic tools employed before someone finally said “we noticed your eye flickering and that’s from BPPV. Here’s meclizine to take.” (That “flickering” is nystagmus.)
That was the treatment provided. No referral to PT for the Hallpike-Dix to evaluate and the Epley maneuver to treat. Just meds after throwing the kitchen sink of imaging at her. I did tell her when she texted me from the hospital that her texted symptoms sounded like BPPV…. 🙃
There are more than four million U.S. ED visits annually for dizziness or vertigo, costing over $4 billion in yearly workup costs. A meaningful percentage of those patients have BPPV. They're not sick. They're otoliths are out of their normal position. But we keep charging them (and the system) a fortune in imaging, overnight stays, and specialist consults, while a frightened patient waits days for an answer a ten-minute bedside test could have given them in the ER.
The otoliths just need repositioning. So does the medical approach to evaluating and treating them.
Career Moves
What are you doing between now and your next career after direct patient care?
For the clinicians who have a gut feeling or even know they will transition away from the bedside “at some point,” take heart! You can start preparing today. Preparing before you want to leave or are ready to leave direct patient care can make it so much easier when it’s time to plan your transition.
Here are a few things you can do right now as a starting point.
Build your professional reputation. Your reputation is one of the most portable assets you have. It travels with you outside the clinic or organization’s walls. Start by showing up consistently and being known for something beyond your clinical role. That might mean volunteering to precept students, joining a committee, presenting at a staff meeting, or contributing to a policy update.
In my case, I was first known for being an expert in managing the throughput of fragile patients from hospital through post-acute settings to home safely. That led to me as the obvious choice to help lead the development and implementation of a transitions of care program and team.
Outside your workplace, think about LinkedIn. If you don't have a profile, create one. If you have one, dust it off. Don't announce anything. Just start connecting with colleagues, sharing the occasional insight from your clinical experience, and engaging with content in spaces you're curious about. Add value to others. Set a cadence for interacting on Linked In. Three times per week is a good starting point.
The goal right now isn't to job hunt. It's to make sure that when opportunities come up, people already know who you are
Unsure what’s valuable to learn about? Start by reading industry journal and blogs. One of the biggest barriers clinicians face when exploring non-bedside roles is not knowing what skills or experience actually translate. The good news is you can start closing that gap just by reading.
Pick one or two journals, newsletters, or blogs in an area that interests you, whether that's health tech, care management, informatics, policy, or something else entirely. Start consuming content. You're getting familiar with the language, the problems people are trying to solve, and the conversations happening in that space.
As you read, you'll start to notice things. You'll recognize gaps that your clinical perspective could speak to. You'll see job titles you've never heard of. You'll come across skills that keep coming up. Start a running list.
This is low-stakes intel gathering that costs nothing but a little time. It’s a great investment.
Here are a bunch of suggestions for journals, publications, and news sources to check out. Check them out and pick a few. If I were choosing three to call mandatory, they would be a., e., and k.:
Health Affairs (especially Forefront)
JAMA Network, especially health policy and informatics pieces
CMMI newsletters: sign up for email updates at this link
Newsletters I recommended at the top of this article
Start managing what you learn. Reading is only half the equation. What you do with what you read is where the real value builds.
This is where personal knowledge management comes in. In simple terms, it's a system for capturing, organizing, and revisiting what you're learning — so it doesn't just disappear after you close the tab.
Start small: when something you read resonates, write a few sentences about it in your own words and save it somewhere intentional. A notes app, a doc, a dedicated notebook—whatever you'll actually use.
Here's why this matters more than it might seem at first:
When you take notes in your own words, you're not just saving information. In fact, the point is to not just save information. The valuable part is that you're processing it.
You start connecting ideas across different articles. You begin forming opinions. And over time, you develop a point of view that is uniquely yours and shaped by both your clinical experience and your growing knowledge of the industry you want to move into.
That point of view is what makes you valuable outside the clinic. It's what gives you something to say in an interview, something to write about, something to share with a colleague.
It also helps you stand out. When you start the job search for your first non-clinical role, this may be the most important tool in your toolbox. It 100% was for me.
I wrote about personal knowledge management here.
This Week, Try This
I co-host a relatively niche podcast on the “future of physical therapy,” aptly named Future Proof PT. The most recent episode, Episode 27, is about AI in Healthcare. It’s for any clinical or clinically-adjacent audience. My cohost Alex Bendersky and I have a chat with Sergei Polevikov.
Check it out the episode here:
Here’s a “short” from the episode that’s under 60 seconds:
*Disclaimer: All opinions and ideas expressed in this article are solely mine and none represent a recommendation or should be viewed as advisement of any kind to anyone to do anything.*


Reply